 Amazingly we are born with 300 bones but over time some of them along with cartilage fuse together until just 206 remain to adulthood.
Amazingly we are born with 300 bones but over time some of them along with cartilage fuse together until just 206 remain to adulthood.
Bone is a living, growing tissue that is forever changing but easily taken for granted. It’s often not until we stub our toe, suffer a fracture or shin splint that we even register their importance to our life, mobility and freedom.
What is bone?
Bone is mostly made from the protein collagen, which keeps bone flexible, and the mineral calcium phosphate which keeps bones strong.
Phosphorus, Vitamin A, D and C, magnesium and fluoride are also important bone nutrients with most being found in foods such as milk products, fish, beans, whole grains and leafy green vegetables.
Bone is constantly on the move..
Bones undergo constant renovation, with old bones being replaced by new. This process involves a balance between the activity of osteoclasts, which break bone down, and osteoblast, which reform and rebuild bone. A change in the balance can lead to losses or gains in bone mass and mineral content. Despite this we are constantly remodelling and regenerating our bones around 10% every year.
Around 99% of the calcium in your body is stored in your bones and teeth, providing strength. The remaining 1% is in the blood and soft tissues where it helps to regulate nervous impulses, muscle contraction and certain enzymes.
To maintain adequate calcium the body requires a constant supply. When this is not provided by the diet, calcium will be removed from the stores in bones. Insufficient calcium intake to promote bone growth during childhood through to puberty can contribute to stress fractures (broken bones) in the short term and osteoporosis (thinning of bone) in later life
The importance of peak bone mass
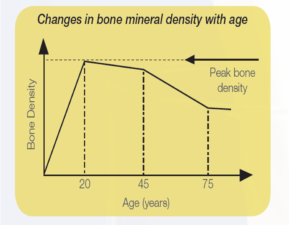
The time just before puberty is extremely important, as this is the time when bone is accumulated. Peak bone mass (density) is achieved between the ages of 20-30 years, following which in both men and women there is an age-related decline in bone mass (see diagram below). For most of us bone loss can be significantly slowed through good nutrition and exercise
 Hormonal changes and groups at risk
Hormonal changes and groups at risk
Young people and athletes
The development of bone density or strength that increases during childhood is aided by growth and sex hormones. Ninety percent of peak bone mass is reached around 18 years in girls and 20 years in boys.
Young women in endurance sports, gymnasts and ballet dancers, who lower their energy intake or body fat to minimum levels in an attempt to control weight, are at particular risk of bone loss. They may develop athletic amenorrhoea (menstrual irregularity) in which periods may be late to start, or lost for three months or more. This can not only lead to a loss of calcium causing bone fragility but also results in failing sports performance and health.
Boys can also be at risk of falling bone density and eating disorders if they are overtraining and undereating. Athletes at risk include those involved in weight- categorised sport, such as equestrian, wrestling, lightweight rowing and endurance.
Adults as they age
Loss of body weight due to overtraining and undereating can affect adults at any age.
In women, bone loss increases rapidly after menopause, when oestrogen levels fall. Because oestrogen protects bone, anytime there is a drop in oestrogen bone loss will follow.
Men can also experience bone loss as testosterone levels naturally start to fall around 30-40years.
Low testosterone can also be associated with some cancer treatments, mumps, haemochromatosis etc as well as secondary causes such as obesity, pituitary disorders, trauma and stress etc.
Not only a person’s hormone levels but also their genetics, and lifestyle factors such as diet and activity determine their peak bone density, bone strength and thus the risk of osteoporosis.
Osteoporosis
Osteoporosis is a condition where the structure of the bone has been weakened, bone begins to thin which increases the risk of bone fractures.
Risk factors for Osteoporosis
- Genetics
– Family history (mother/grandmother)
– Being Caucasian (fair skinned) or Asian
- Nutritional factors
– Low calcium intake from diet
– High alcohol intake
– Excessive salt (sodium) intake
– A high intake of protein
– Excessive caffeine intake
- Lifestyle factors
– Insufficient weight bearing exercise
– Cigarette smoking
- Other factors – to refer to your doctor
– Early menopause or ovaries removed
– Menstrual cycle irregular or stopped
– Some medications e.g. steroids
Tips for optimal bone health
While genetics do play a role in developing osteoporosis a person can greatly minimise risk and build stronger bones throughout life in the following ways:
Exercise
For adults the best exercise to build strong bones involves placing a force on the bones. This may be the force of gravity or that of contracting muscle (muscle pull). As such it is weight bearing exercise or strength training that is most beneficial to adults. These types of activities stimulate the building of new bone and slow the loss of bone so that they are better able to cope when loads are applied. Consequently well trained athletes have a higher bone mass than those people who are inactive.
Swimming and cycling are less effective in building strong bones. Activities involving walking, running, and jumping are all appropriate weight bearing exercises to aid bone health. Postmenopausal women may also find strength training can be effective.
For children bone strengthening activities not only help bones but also strengthen muscles and aerobic health. These could include: Hopscotch, hopping, skipping, bouncing on a trampoline, climbing trees and hanging from jungle gyms at school. Running and sports like gymnastics, basketball and volleyball also help.
Older children and teenagers who are still growing should avoid powerlifting, body building and maximal lifts or exercises that attempt to build excess muscle mass while bone is still growing. Structured resistance or strength training (and circuit training) using exercise bands, hand-held weights and weight machines (set at low calibrations), as part of a supervised sports program or generally to increase their strength, can be a safer option.
Maintain a healthy weight
Calcium has also been shown to have a role in weight management, with those eating lower energy but high calcium containing foods being more successful in losing weight than those who limit calcium. Additionally foods that are good sources of calcium such as milk and yoghurt have a lower Glycaemic index therefore promoting greater satiety over a longer period of time. A dietitian can advise you about safe weight management (gain or loss) if so required.
Consume sufficient calcium
Achieving an adequate calcium intake is the most important nutritional factor in maximising bone mass. The recommended daily intake (RDI) as shown below reflects our different needs through the life cycle.
NB:Calcium obtain from eating whole foods is better absorbed than when taken as calcium supplements. Be guided by your GP.
Calcium requirements for different age groups
| Groups | Age | Calcium (mg/day) |
| Infants | 0-6 months | 210 |
| 7-12months | 210 | |
| Children | 1-3 years | 500 |
| 4-8 years | 700 | |
| 9-11 years | 1000 | |
| 12-13 years | 1300 | |
| Men | 19 years plus | 1000 |
| Women | 19-50 years | 1000 |
| 51 years plus | 1300 | |
| Pregnant | 14-18 years | 1300 |
| 19 years plus | 1000 | |
| Breast feeding | 14-18 years | 1300 |
| 19 years plus | 1000 | |
| Aust/NZ RDI 2006 |
Avoid calcium inhibitors
Other nutritional factors, such as excess intakes of salt (sodium), protein, dietary fibre and caffeine, alcohol and cola drinks (that is, containing phosphoric acid) tannins and phytates can all increase the loss of calcium in urine, but have the most effect when a person has a poor calcium intake as well..
If you would like to undertake a dietary assessment of your bone nutrients then contact me today
For more information on how calcium inhibitors can be controlled, practical ideas for increasing calcium intakes on a daily basis and references for this article read:
How to Grow an Athlete: From Playground to Podium -Lea’s latest book see website to purchase
Articles by Lea on this subject
Children’s bone and gut health are linked
Osteoporosis the silent disease
Healthy diet aids menopause treatment
Overcome misconceptions about weight for better family health






























































Leave a Reply